37 million people live with HIV worldwide and all of them need access to life-saving anti-retroviral treatment. UNAIDS has given us a roadmap in how an ‘end to AIDS’ can be achieved by 2030. One of its core elements is the so-called 90/90/90 treatment concept which needs to be realized by the year 2020 in order to put an end to AIDS as a public health threat by 2030: 90% of people living with HIV should know their HIV-status, 90% of those who test positive should be on treatment and 90% of those on treatment should have an undetectable viral load, i.e. be on successful and effective anti-retroviral treatment.
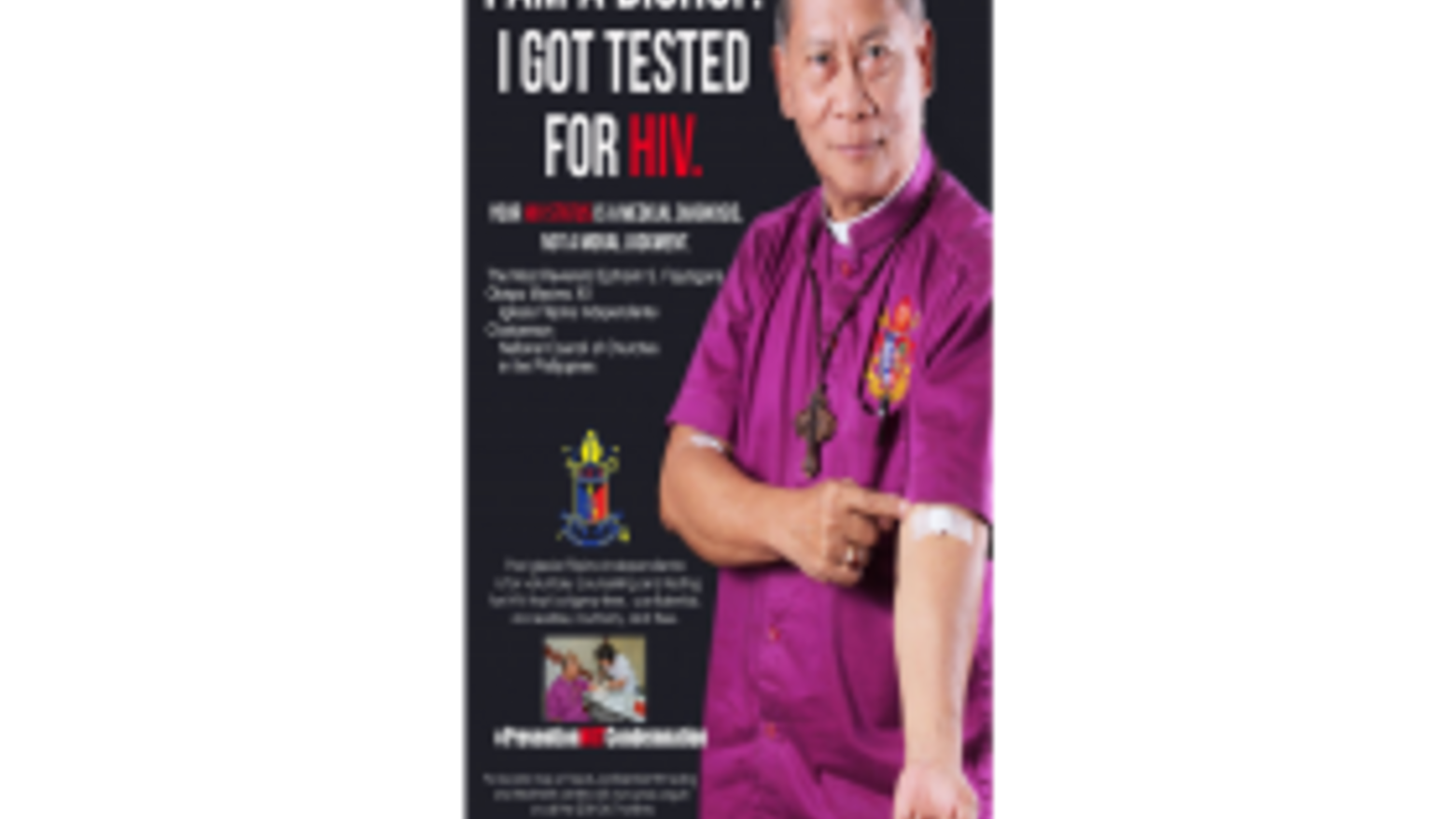
The first 90% is a big challenge. At present, less than 50% of people living with HIV know their HIV status. How can people be motivated to go for HIV testing? The National Council of Churches in the Philippines used a strategy that has worked elsewhere – the collaboration with well-known people – in this case clergy. The photos of leading bishops who have gone for an HIV test are shown on posters to inspire others to undergo an HIV test as well. So far the main HIV data in the Philippines is from the MSM (men having sex with men) and the PWID (people who inject drugs) communities. It will therefore be interesting to see, if this campaign gets the general population to test as well. The Philippines are a country where incidence is rising dramatically – from one new infection every 3 days in the year 2000 to 9 new infections per day in the year 2012 to 22 new infections per day in 2015. Yet the data is very limited because so few people have tested. Working with well-known clergy seems a promising way forward and it will be interesting to get the results of this campaign in a few months’ time.
This strategy could and should be used globally and the faith communities could play a leading role here – imagine the Pope on a poster saying he’s just tested for HIV! Would that not inspire millions of people to do the same? And this strategy might also help to have more men come forward for testing. At present the vast majority of people who test are women. Men have lower access to anti-retroviral treatment than women and a higher death rate due to HIV complications. So strategies need to be developed to get more men to test and be treated early. For men to wait until their immune system is seriously compromised before they seek medical help is life-threatening.
But we also need functional health systems which are able to put and maintain more people on anti-retroviral treatment and we need viral load machines to monitor treatment effectiveness. There are few viral load machines available in countries of the Global South, as the machines and tests are too expensive. We need the tests to come down to about 5 US Dollars to enable countries to follow the new WHO treatment recommendations: to put people on treatment as soon as they are diagnosed HIV-positive and to do regular viral load tests to see that they have an undetectable viral load within the space of 6 months after commencing treatment and keep suppressing the virus. If the viral load rises again one needs to check, if this is due to poor adherence or if the medicines do not work anymore because of resistance. If the latter is the case, the HIV-positive person needs to receive a different treatment regimen. It is only by monitoring people on treatment closely and having access to 2nd and 3rd line anti-retroviral treatment that we can assure lifelong treatment for all people living with HIV.
In 2015 about 15 million people had access to anti-retroviral treatment – an impressive number of people but only 41% of those who need to be treated. So let us not be complacent and stop half-way on the road to end the epidemic. Let us re-double our efforts to get everyone who is HIV-positive to know their status and to be on effective treatment but let us also re-double our fight against stigma and roll out evidence-based prevention measures.
New infections need to be brought down from presently 2 million per year to 500.000 by the year 2020 and 200.000 by the year 2030, if we want to end the AIDS epidemic. After years of educating people on HIV, only 35% of youth have comprehensive knowledge on HIV. Many more efforts need to be made to pass on correct knowledge, to talk openly about sexuality and condom use in and out of schools, in communities, sports clubs, churches, etc. and to de-stigmatize HIV. It has to be normal to go for an HIV-test locally and to access treatment locally. While people are still prepared to travel long distances out of fear to be seen at a local health centre associated with HIV services, we will hardly make an inroad on prevention and treatment.
We continue to need more financial resources. The German Government should finally increase the contribution to the Global Fund substantially in order to support effective treatment programmes in low and middle income countries. Germany, one of the leading world economic powers should follow the example of the US and the UK - countries which make substantial contributions to global health and the global response to HIV.
We also need cheaper diagnostics. The producers of viral load machines should lower the prices for the machines and reagents substantially so that countries are able to roll out viral load testing. But we also need NGOs and churches to combat stigma effectively, to roll out evidence-based prevention programmes and to collaborate closely with HIV-positive people and with community, political and church leaders in order to inspire men and women and adolescent girls and boys to go for testing and to be inclusive as a community. The Philippines have set a good example, are we all prepared to follow?